Prince Albert Piercing: Everything You Need to Know About the Most Popular Male Piercing

Making the decision to acquire a male genital piercing requires both courage and a deep understanding of human anatomy. Among all available options, the Prince Albert (PA) piercing stands out as the most widely requested, bridging the gap between aesthetic enhancement and functional stimulation. Before undertaking any modification of this caliber, it is imperative to approach the subject with clinical objectivity. This chapter demystifies the anatomical realities of the procedure, establishing a foundation of medical accuracy and procedural safety.
Prince Albert Piercing: Everything You Need to Know About the Most Popular Male Piercing
From a clinical standpoint, the Prince Albert piercing follows a highly specific and remarkably efficient anatomical pathway. The procedure is defined by an insertion point that enters directly into the urethral meatus—the natural opening at the tip of the penis. From inside the fossa navicularis (the widened portion of the urethra situated within the glans), the piercing needle is guided downward to exit through the ventral side, which is the bottom or underside of the glans.
This exit point is typically located just alongside or perfectly centered at the base of the frenulum, where the head of the penis meets the penile shaft. The tissue traversed by the needle consists primarily of the corpus spongiosum, a highly vascularized spongy tissue that surrounds the urethra. Because the internal portion of the piercing rests against the urethral mucosa—a specialized mucous membrane designed to continuously flush out bacteria via urination—the Prince Albert boasts an exceptionally rapid cellular turnover rate. This unique biological advantage makes it one of the fastest-healing body modifications available, provided the exact anatomical placement is executed with surgical precision. Improper placement that bites too deeply into the vascular tissue or too shallowly near the surface can lead to complications, underscoring the necessity of professional execution.
Anatomical Requirements and Considerations for Circumcised vs. Uncircumcised Clients
While the core mechanics of the piercing remain consistent, variations in external male anatomy dictate crucial adjustments in technique and jewelry selection. The presence or absence of the prepuce (foreskin) drastically alters the biomechanical environment of the glans and how the piercing will heal and function daily.
For circumcised clients, the absence of the foreskin means the glans is continuously exposed to external friction from clothing. The tissue of the glans is highly keratinized (toughened), and the piercing’s entry and exit points are openly visible. In these cases, the piercer must carefully measure the diameter of the corona to ensure the jewelry ring sits flush against the skin without applying undue pressure on the underside of the shaft, which could lead to tissue migration over time.
For uncircumcised clients, the anatomical dynamics shift. The foreskin provides a natural, protective pocket that keeps the glans moist and shields the piercing from external friction during the initial healing phases. However, the piercer must meticulously account for the gliding motion of the foreskin. The placement and jewelry size must accommodate the full retraction of the prepuce over the glans to prevent the jewelry from catching, pinching, or tearing the delicate mucosal tissue. Furthermore, uncircumcised clients require specialized hygiene education to ensure the enclosed environment does not trap lymphatic discharge or natural secretions around the fresh puncture wound.

Prince Albert Piercing
The Importance of a Sterile Environment: Why Expertise Matters at pinktatpier
Genital piercings naturally evoke a heightened sense of vulnerability and apprehension. Recognizing this psychological and physical reality, pinktatpier has engineered an environment that strictly adheres to the highest echelons of clinical hygiene and professional conduct. Operating as a completely sterile, judgment-free zone, the studio is designed to eliminate client anxiety through unwavering expertise and transparency.
At pinktatpier, the mitigation of cross-contamination and infection is our paramount directive. The studio employs hospital-grade autoclaves for the sterilization of all non-disposable implements, while utilizing strictly single-use, specialized piercing needles that are unsealed in front of the client. The surrounding environment is maintained with medical-grade surface disinfectants to neutralize airborne and contact pathogens. Furthermore, our specialists operate with bedside manners akin to medical professionals. Every step of the procedure is narrated calmly and clinically, ensuring you are never caught off guard. Choosing a specialist at pinktatpier guarantees that your procedure is not treated as a mere aesthetic service, but as a precise anatomical modification performed with absolute respect for your health and comfort.
Pre-Procedure Consultation: What to Expect During Your Initial Clinical Evaluation
The hallmark of a safe and successful Prince Albert piercing is the rigorous assessment that occurs before a needle is ever prepared. The experts at pinktatpier perform a strict anatomical consultation prior to any male piercing to ensure the client is a viable and safe candidate.
During this mandatory evaluation, the piercer conducts a visual and tactile assessment of the genital anatomy. We evaluate the elasticity of the tissue, the prominence and tension of the frenulum, and the structural integrity of the urethral meatus. Not every anatomy is universally suited for a standard PA piercing ; conditions such as hypospadias (where the urethral opening is not located at the tip) or an exceptionally tight frenulum (frenulum breve) require specialized consideration or may disqualify a client from receiving this specific placement safely. Our experts will transparently discuss your unique vascular structure and map out the safest trajectory for the needle to avoid major blood vessels. This preemptive clinical diligence ensures that when you proceed with the piercing, the risk of excessive bleeding or anatomical rejection is virtually eliminated.
Prince Albert vs. Reverse PA Piercing: Key Anatomical Differences
| Feature | Prince Albert Piercing (Standard PA) | Reverse Prince Albert Piercing (RPA) |
| Entry Point | Inside the urethral meatus | Inside the urethral meatus |
| Exit Point | Ventral side (bottom) of the glans, near the frenulum | Dorsal side (top) of the glans, near the corona |
| Tissue Traversed | Corpus spongiosum (underside) | Corpus cavernosum / thicker dorsal tissue |
| Healing Speed | 4 to 8 weeks (generally faster) | 4 to 6 months (significantly slower) |
| Common Jewelry | Captive Bead Ring, Curved Barbell, Circular Barbell | Curved Barbell, specialized Prince’s Wand |
Managing Expectations: Prince Albert Piercing Pain and Initial Bleeding
The anticipation of a genital modification frequently generates profound psychological distress, primarily centered around the fear of extreme pain and uncontrollable hemorrhage. However, clinical realities diverge significantly from these common anxieties. This chapter systematically dissects the physiological responses associated with the procedure, equipping clients with the critical knowledge necessary to navigate the initial days post-piercing. By understanding the body’s natural mechanisms, clients can approach the experience with total confidence rather than trepidation.
The Pain Reality: Why Prince Albert Piercing Pain is Clinically Lower Than Expected
The absolute most pervasive deterrent for men considering this modification is the assumption of agonizing, unbearable pain. In reality, Prince Albert piercing pain registers surprisingly low on the clinical discomfort scale, especially when systematically compared to denser tissue modifications like ear cartilage or nipple piercings. Cartilage involves puncturing rigid, avascular connective tissue, resulting in a prolonged, dull ache and an extended, highly sensitive inflammatory response. Conversely, the highly specialized genital tissue involved in this procedure is exceptionally pliable, accommodating, and designed for rapid natural dilation.
The sensation is frequently described by our clients as a brief, sharp pinch followed immediately by a localized sensation of dull pressure, rather than excruciating agony. Because the tissue is incredibly thin at the precise point of perforation, a master piercer can execute the precise needle maneuver in a fraction of a second. Furthermore, the localized nerve endings in this specific region respond to the swift, highly controlled trauma with an immediate, massive surge of endorphins, acting as a powerful natural analgesic. This innate biological response drastically blunts the nervous system’s perception of the sensation, meaning the mental anticipation is unequivocally worse than the actual, fleeting physical moment of the puncture.
The Bleeding Phase: Understanding Normal Post-Procedure PA Piercing Bleeding
Following the incredibly brief moment of perforation, the body immediately initiates its natural hemostatic response to seal the channel. It is absolutely crucial to understand that PA piercing bleeding is a standard, fully expected clinical outcome and fundamentally not an indicator of a botched procedure. The male genital region is densely packed with a rich, highly active network of micro-vessels strictly necessary for normal biological function. When these vessels are cleanly severed by a piercing needle, they will bleed, and due to the heavy vascularity, it frequently appears more voluminous than a standard earlobe or facial piercing.
This initial bleeding phase typically reaches its peak within the first twenty-four hours. It is highly common for fresh blood to mix with normal lymphatic fluid and urine, which can sometimes make a minor amount of blood look like a significantly larger, more alarming volume due to simple liquid dilution. The most effective, hygienic, and clinically recommended method for safely managing this phase is the strategic use of breathable, sterile gauze pads or unscented sanitary panty liners placed directly inside the client’s underwear. This simple containment strategy isolates the fluid, protects your clothing, and provides gentle, passive pressure against the fresh wound site, thereby encouraging rapid blood coagulation without suffocating the healing tissue.
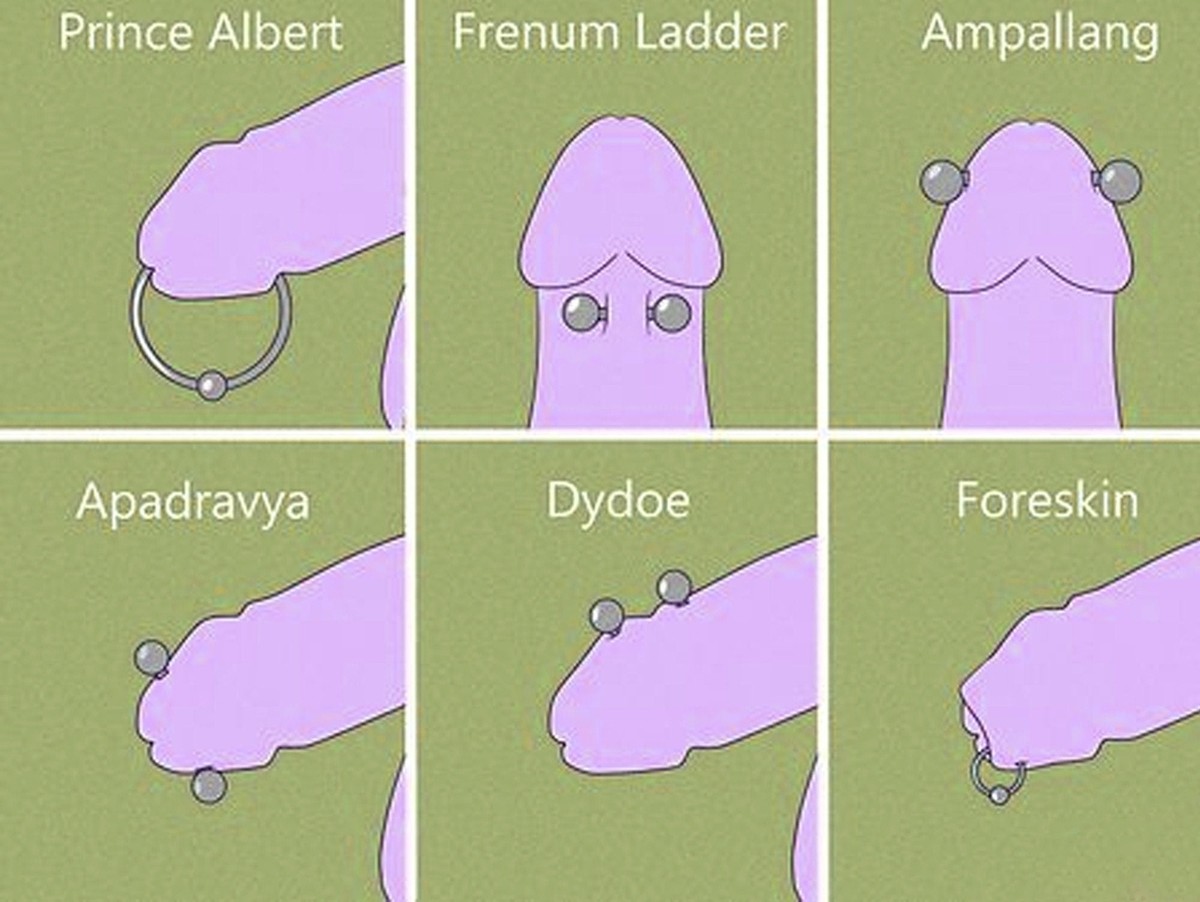
Prince Albert Piercing
Immediate Clinical Care: pinktatpier’s Protocols for Minimizing Post-Procedure Discomfort
The transition from the initial puncture to the final jewelry insertion is the most critical window for proactive pain management. At pinktatpier, our seasoned specialists deploy advanced procedural protocols specifically engineered to minimize tissue trauma and eliminate client distress. We utilize precisely calibrated receiving tubes that act as a strict physical barrier, protecting surrounding sensitive tissues from unintentional needle contact while guiding the puncture with absolute, flawless geometric accuracy.
Our piercers are rigorously trained in the highly technical art of the swift needle-to-jewelry transfer. The sterile jewelry follows the hollow needle seamlessly in one continuous, perfectly fluid motion. This elite clinical technique prevents the fresh wound channel from collapsing and immediately seals the puncture, drastically reducing both the Prince Albert piercing pain and the initial, immediate surge of PA piercing bleeding. Throughout this highly choreographed sequence, the pinktatpier specialist expertly guides the client through specialized parasympathetic breathing exercises—syncing a deep inhalation and forceful exhalation with the exact microsecond of tissue perforation. This psychological and physiological anchoring actively lowers the heart rate, mitigates the involuntary physical flinch response, and ensures a smooth, highly controlled environment.
At-Home Management for the First 48 Hours: Compression, Rest, and Containment
Once the client confidently leaves the sterile, reassuring sanctuary of pinktatpier, the primary responsibility of care shifts to diligent, strictly observed at-home management. The overriding directive for the first forty-eight hours is strict physical rest combined with the application of mild, passive compression. Clients are strictly instructed to wear snug-fitting, highly supportive cotton underwear—such as standard briefs or tight boxer briefs—to restrict excessive anatomical movement. Pendulous swinging or repetitive friction against loose fabric will aggressively disrupt the fragile initial blood clot, prematurely restarting the bleeding phase and inducing entirely unnecessary soreness.
During this highly critical window, clients must rigorously avoid ingesting any medications that actively thin the blood, such as aspirin or ibuprofen, unless explicitly directed by a licensed medical professional, as these can severely prolong the necessary clotting process. Furthermore, all strenuous cardiovascular activities, heavy gym lifting, and any form of localized physical trauma must be entirely suspended. By combining strict physical containment with the continued, diligent use of sanitary liners, clients actively facilitate an optimal environment for the tissue to stabilize, transitioning rapidly from a fresh open wound to a safely healing fistula.
First 7 Days Expectation Chart: Normal Bleeding vs. When to Contact a Doctor
| Days Post-Procedure | Normal Clinical Expectations (Standard Healing) | Warning Signs (Require Immediate Medical Attention) |
| Days 1 – 2 | Moderate bleeding, sharp stinging strictly during urination, localized swelling, minor bruising. | Profuse, pulsating bleeding that rapidly soaks through a thick pad in under an hour; inability to stop bleeding with direct pressure. |
| Days 3 – 4 | Light spotting on gauze, mild tenderness, secretion of clear or slightly white lymphatic fluid (sebum). | Spreading, angry red streaks extending up the penile shaft; severe, unrelenting throbbing pain. |
| Days 5 – 7 | Minimal to zero bleeding, slight crusting on the jewelry ring, dull ache only if bumped or snagged. | Thick, foul-smelling yellow or green pus; localized heat; systemic fever; complete inability to pass urine. |
Prince Albert Jewelry Guide: Sizing, Materials, and Styles
Selecting the appropriate hardware for a male genital modification transcends mere aesthetic preference; it is a fundamental biomechanical decision that dictates the safety, structural integrity, and success of the entire healing process. The physical environment of the lower anatomy subjects any inserted foreign object to constant friction, gravity, and localized pressure. Consequently, understanding the clinical mechanics behind Prince Albert jewelry is paramount. This chapter outlines the strict metallurgical and physical standards required to ensure your modification heals flawlessly and remains structurally sound for a lifetime.
Initial Gauge Sizes: Starting Thick to Prevent Rejection and the “Cheese-Cutter” Effect
One of the most critical clinical errors in male genital piercings is initiating the procedure with a wire diameter (gauge) that is excessively thin. In standard body modifications, such as earlobes or facial cartilage, thinner gauges like 14g (1.6mm) or 16g (1.2mm) are customary. However, applying these delicate sizes to a PA piercing introduces a severe biomechanical hazard universally referred to in the clinical piercing community as the “cheese-cutter effect.”
This phenomenon operates on a basic principle of physics: force divided by area equals pressure. When a very thin ring is inserted through the mucosal tissue of the lower glans, the concentrated weight of the metal—combined with the natural pull of gravity and daily movement—creates immense, highly localized pressure on the underside of the urethral tract. Over time, this thin wire acts precisely like a wire cheese slicer, slowly migrating downward, necrotizing the surrounding cellular walls, and systematically tearing through the tissue.
To completely neutralize this risk, the specialists at pinktatpier mandate an initial piercing size of either 10g (2.5mm) or 8g (3.2mm). While starting at a thicker gauge may sound counterintuitive to an anxious client, it is actually the clinically superior, safer, and far more comfortable method. A thicker piece of Prince Albert jewelry substantially increases the surface area that rests against the tissue. This disperses the weight and mechanical stress evenly across a wider section of the wound channel, stabilizing the piercing , eliminating the risk of downward migration, and preventing microscopic tearing during physical activity.

Prince Albert Piercing
Material Matters: The Absolute Necessity of Implant-Grade Titanium
The metallurgical composition of your initial jewelry is just as critical as its physical dimensions. When an open wound is created, the body’s immune system immediately begins assessing the foreign object placed inside the newly formed channel. To ensure rapid cellular synthesis and prevent severe immunological rejection, the material must possess total biocompatibility. This is why the absolute necessity of Implant-Grade Titanium (specifically ASTM F-136 compliant) cannot be overstated.
Many standard piercing studios utilize 316L Surgical Steel, which, despite its clinical-sounding name, is fundamentally an alloy that contains trace amounts of nickel. In the highly vascularized, moist environment of a fresh urogenital puncture, the acidic nature of bodily fluids and urine can cause steel to microscopically degrade, leaching nickel directly into the bloodstream. This frequently triggers localized allergic contact dermatitis, presenting as severe itching, prolonged swelling, and excessive fluid discharge that severely complicates healing.
Implant-Grade Titanium, conversely, is entirely hypoallergenic, non-porous, and completely nickel-free. It is the exact same ultra-pure metallurgical standard utilized by orthopedic surgeons for bone screws and joint replacements. Furthermore, titanium develops a natural, microscopic oxide layer that prevents the adherence of bacteria and organic cellular debris to the jewelry’s surface, keeping the puncture site dramatically cleaner. As an added biomechanical benefit, titanium is roughly forty-five percent lighter than steel, significantly reducing the gravitational pull on the fresh tissue and enhancing overall comfort during the initial weeks.
Captive Bead Rings vs. Curved Barbells: Selecting Your Initial Prince Albert Jewelry
Once the proper gauge and material are established, clients must choose the physical geometry of their initial Prince Albert jewelry. The two clinically approved styles for a fresh procedure are the Captive Bead Ring (CBR) and the Curved Barbell, each offering distinct biomechanical advantages depending on the client’s specific anatomical structure and lifestyle requirements.
The Captive Bead Ring is universally recognized as the gold standard for initial placement. Its circular geometry allows for smooth, continuous rotation through the fistula (the healed piercing channel). This rotation is highly advantageous during the initial healing phase because it prevents lymphatic fluid and natural crusting from adhering the metal statically to the tissue. Furthermore, a properly sized ring accommodates standard post-procedure edema (swelling) without compressing the newly traumatized area.
Alternatively, a Curved Barbell offers a more streamlined, fixed profile. Because it consists of a curved post with a bead at either end, it does not complete a full circle and therefore minimizes bulk. This can be clinically beneficial for clients who engage in rigorous, high-impact athletic activities where a ring might catch or snag on athletic support garments. However, barbells are generally less forgiving regarding initial swelling. A highly trained professional must carefully measure the exact length of the barbell post to ensure adequate extra room is left for the tissue to expand safely during the first vital days of the inflammatory response.
Upgrading Your Jewelry: Clinical Timelines for Safely Changing Your Piece
Patience is the ultimate virtue when transitioning from your initial, clinical-grade hardware to more stylized, permanent pieces. Attempting to remove or alter the jewelry before the fistula has established a robust, highly keratinized internal wall will instantly tear the fragile new cells, reverting the healing process back to day one and introducing a massive risk of localized infection.
Clients must strictly wait a minimum of eight to twelve weeks before attempting any aesthetic changes. When the clinical timeline has been met, you are encouraged to return to the studio to explore the expansive pinktatpier jewelry collection. Our specialists will perform a sterile, professional swap, utilizing specialized taper tools to seamlessly guide the new piece into the channel without causing microscopic internal abrasions. Upgrading safely ensures that your piercing transitions from a medical procedure into a comfortable, permanent enhancement.
Standard PA Jewelry Gauge Sizes & Styles (CBRs vs. Barbells)
| Feature | Captive Bead Ring (CBR) | Curved Barbell | Circular Barbell (Horseshoe) |
| Geometry | Fully closed circle with a tension-held bead. | Arced post with threaded beads on both ends. | Open semi-circle with threaded beads on both ends. |
| Initial Gauge | 10g (2.5mm) or 8g (3.2mm) | 10g (2.5mm) or 8g (3.2mm) | 10g (2.5mm) or 8g (3.2mm) |
| Healing Benefit | Excellent accommodation for swelling; easy to clean. | Minimal profile; less prone to catching on fabric. | Combines the benefits of a ring with easy removal. |
| Migration Risk | Lowest risk due to equal weight distribution. | Moderate; requires precise length measurement. | Low risk; weight is balanced evenly on both ends. |
Male Piercing Aftercare: Navigating the PA Piercing Healing Time
The successful integration of a male genital modification is not solely dependent on the skill of the practitioner; it relies heavily on the client’s strict adherence to clinical aftercare protocols. Once you leave the sterile, controlled environment of pinktatpier, the responsibility of maintaining tissue health transitions entirely to your daily routine. This chapter outlines the precise, medically sound practices required to navigate the healing phase safely, ensuring your modification matures without immunological complications, localized infections, or structural setbacks.
The Healing Timeline: Clinical Milestones in the First 4 to 8 Weeks
When evaluating the PA piercing healing time, clients are frequently surprised to discover that this specific modification boasts one of the most rapid recovery trajectories in the entire body art industry. Because the piercing traverses the highly vascularized corpus spongiosum and the continually flushed urethral mucosa, the localized cellular turnover rate is exceptionally high. Generally, the primary PA piercing healing time spans a mere four to eight weeks, provided strict hygiene and physical containment protocols are maintained.
The healing process is categorized into three distinct clinical phases. The initial inflammatory phase (days one to seven) involves the body’s natural hemostatic response and localized edema. Following this is the critical proliferative phase (weeks two through four), where the body aggressively synthesizes new epithelial cells to line the puncture wound, creating the foundational fistula (the permanent internal channel). Finally, the maturation phase (weeks five through eight) fortifies this delicate cellular wall, transforming it into robust, toughened tissue capable of withstanding standard daily friction and anatomical movement.
Daily Cleansing Protocols: Sterile Saline Soaks and the Natural Cleansing Effect of Urine
The clinical foundation of cleaning a Prince Albert piercing relies on biological harmony rather than chemical warfare. The primary external cleaning agent should exclusively be a sterile, packaged isotonic saline solution (0.9% sodium chloride). This exact ratio flawlessly mimics the body’s natural osmotic balance, allowing you to flush away cellular debris without aggressively dehydrating or shocking the newly formed epithelial cells. At pinktatpier, we strongly advise clients to perform a dedicated saline soak twice daily—once in the morning and once in the evening. This is achieved by gently submerging the glans in a clean, medical-grade or disposable cup of warm saline for exactly three to five minutes.
Internally, the piercing benefits from a fascinating and highly efficient biological advantage: the natural cleansing effect of urination. While human urine is not perfectly sterile once it reaches the lower urethra, it originates sterile in the bladder and possesses a mildly acidic pH. As it forcefully passes through the urethral tract and washes over the internal jewelry mechanism, it acts as a powerful, natural physiological flush. This constant, daily irrigation effectively clears away microscopic debris, dead cellular matter, and potential bacterial colonies from the internal wound channel. Therefore, maintaining excellent hydration by drinking ample water throughout the day is a critical, proactive component of cleaning a Prince Albert piercing.

Prince Albert Piercing
Hygiene Red Flags: Harsh Chemicals, Submerged Water, and What to Strictly Avoid
The most common clinical setbacks encountered during the primary healing phase are directly linked to over-cleaning or environmental contamination. The absolute strictest prohibition during your recovery involves submerged bodies of water. Clients must entirely avoid public pools, communal hot tubs, natural lakes, oceans, and even private bathtubs for a minimum of eight consecutive weeks. These environments are densely populated with aggressive waterborne bacteria, harsh chemical irritants (like chlorine), and microscopic pathogens that can instantly colonize the fresh puncture wound, leading to severe localized infections.
Furthermore, the application of harsh chemical agents is strictly forbidden. The use of standard antibacterial soaps, rubbing alcohol, hydrogen peroxide, iodine, or heavily fragranced body washes will immediately necrotize newly formed, fragile skin cells. These chemicals aggressively strip the tissue of its natural, protective lipid barrier, severely prolonging the healing timeline and inducing agonizing chemical burns. During a daily shower, allow warm, clean water to passively run over the area to rinse away sweat, but never apply lathered soap directly to the entry or exit points of the piercing.
Monitoring the Piercing Site: Differentiating Between Normal Lymphatic Fluid and Infection
As the body actively repairs the channel, it will naturally excrete a clear, slightly white, or pale yellow substance known as lymphatic fluid (sebum). When this fluid contacts the air, it oxidizes and crystallizes on the exposed jewelry, forming hard, crusty deposits. This is a completely normal, healthy physiological byproduct of the proliferative phase and should never be forcibly picked, scratched, or chipped away dry, as doing so will instantly tear the underlying microscopic tissue. Instead, allow the warm daily saline soaks to dissolve these crusts naturally.
It is medically vital to differentiate this healthy biological secretion from a true clinical infection. If the localized discharge transitions into a thick, foul-smelling, dark yellow or green pus, accompanied by severe radiating heat, escalating throbbing pain, or systemic symptoms such as a fever, this strongly indicates a pathogenic complication. In the sterile, judgment-free environment of pinktatpier, we encourage absolute transparency and immediate communication. If you ever suspect an anomaly in your healing trajectory, our experts are always available for a clinical evaluation to ensure your anatomy remains safe and healthy.
PA Healing Timeline: Week 1 to Week 8 (Milestones and Restrictions)
| Timeframe | Clinical Milestone | Strict Lifestyle Restrictions |
| Week 1 | Inflammatory phase: Hemostasis occurs; initial swelling peaks and begins to subside. | No sexual activity; no rigorous exercise; avoid blood-thinning medications; wear supportive underwear. |
| Week 2 – 3 | Proliferative phase: Epithelial cells begin lining the fistula; significant lymphatic fluid excretion (crusting). | No oral contact; no submerged water (pools/baths); continue strictly using only sterile saline for external cleaning. |
| Week 4 – 5 | Maturation phase begins: Tissue feels less tender; crusting minimizes; jewelry moves more freely. | Submerged water still prohibited; protected, gentle sexual activity may be introduced if completely pain-free. |
| Week 6 – 8 | Primary healing concludes: Fistula wall thickens; piercing visually appears fully healed. | Standard activities slowly resume; jewelry downsizing or changing may be assessed by a professional. |
Lifestyle Adjustments: Urination, Intimacy, and Long-Term Care
Integrating a Prince Albert modification into your daily life requires a conscious, methodical adaptation to new biomechanical realities. While the initial recovery phase dictates strict medical protocols, the long-term success of your piercing depends entirely on how you adjust your everyday habits. At pinktatpier, our comprehensive clinical approach extends far beyond the procedure room; we prepare our clients for the practical, everyday realities of living with specialized genital jewelry. This chapter addresses the most significant lifestyle shifts, providing professional strategies for managing altered bodily functions, safely reintroducing physical exertion, and navigating the complexities of intimate contact without compromising the structural integrity of your healing tissue.
Navigating Urination Changes: Practical Tips for Managing the “Sprinkler Effect”
The introduction of a physical metallic object into the terminal end of the urethral tract fundamentally alters the fluid dynamics of urination. Clinically referred to as the “sprinkler effect,” this is an unavoidable, physiological consequence of the Prince Albert piercing . Because the jewelry ring or barbell physically occupies space within the meatus, it aggressively disrupts the natural laminar flow of the urine stream. This disruption forces the fluid to split, fan out, or spray unpredictably upon exit.
For the vast majority of clients, the traditional standing method of urination becomes highly impractical and unhygienic, frequently resulting in soiled clothing or unsanitary bathroom environments. The most effective, universally recommended lifestyle adjustment is transitioning to sitting down while urinating. This simple anatomical shift entirely neutralizes the complications associated with the unpredictable spray, ensuring absolute hygiene and convenience without the daily frustration of collateral splashing.
If standing is absolutely necessary in a public restroom facility, clients must consciously alter their technique. Some men find clinical success by gently rotating the jewelry to temporarily clear the fluid pathway, while others learn to apply mild, strategic pressure to the underside of the urethra to redirect the flow. However, adopting the seated position remains the ultimate, stress-free clinical recommendation by the experts at pinktatpier for long-term daily management.
Resuming Intimacy: Clinical Guidelines for Safely Returning to Sexual Activity
The most frequent inquiry we receive during consultations involves the timeline for safely resuming sexual relations. Patience in this arena is absolutely paramount. Engaging in sexual activity prematurely is the leading cause of severe structural complications, including the microscopic tearing of the delicate fistula, heavy localized hemorrhage, and the introduction of aggressive pathogenic bacteria. Clients must strictly abstain from all forms of sexual contact—including masturbation—for an absolute minimum of four to six weeks.
When clinical healing milestones are successfully met and you are completely pain-free, intimacy may be gradually reintroduced, but it requires strict, non-negotiable protective measures. During the prolonged healing phase (months two through four), the absolute necessity of utilizing a high-quality condom cannot be overstated. A condom serves a dual clinical purpose: it acts as a critical hygienic barrier, preventing the exchange of bodily fluids that could heavily infect the immature wound channel, and it provides a vital mechanical barrier. The latex or polyurethane sheath firmly encapsulates the jewelry, preventing the metal ring or barbell from painfully snagging on a partner’s delicate internal or external tissue. Furthermore, the generous application of a sterile, water-based lubricant is mandatory to eliminate debilitating friction. Silicone-based or oil-based lubricants must be strictly avoided, as they can rapidly degrade latex condoms and trap localized bacteria against the piercing site.
Protective Measures: Managing Friction During Vigorous Physical Exercise and Athletics
For individuals who maintain an active, athletic lifestyle, introducing a genital modification requires deliberate physical containment strategies. Vigorous cardiovascular exercise, heavy weightlifting, and high-impact sports naturally subject the pelvic region to repetitive friction and sudden, ballistic movements. If the jewelry is permitted to swing freely, the constant mechanical pulling will severely traumatize the internal urethral mucosa, leading to microscopic lacerations, chronic inflammation, and drastically delayed healing.
To completely neutralize this kinetic risk, clients must heavily invest in highly supportive athletic undergarments. Standard loose boxer shorts must be entirely discarded in favor of tight-fitting briefs, compression shorts, or specialized athletic jockstraps. The clinical objective is total tissue immobilization. By pinning the anatomy securely against the body, you effectively eliminate the kinetic momentum of the jewelry, allowing you to run, jump, or lift without subjecting the internal fistula to damaging shear forces. Cyclists face a unique biomechanical challenge, as the pressure of a bicycle saddle directly compresses the ventral side of the glans against the jewelry. Extended cycling should be entirely suspended during the primary healing window to prevent localized tissue necrosis or migration.
The Stretching Journey: Safe Anatomical Protocols for Increasing Your Gauge Over Time
As your Prince Albert piercing fully matures over several months or years, you will likely notice the jewelry naturally loosening within the established channel. Because gravity exerts a constant, gentle downward force on the piece, the highly pliable tissue of the corpus spongiosum gradually accommodates the metal. This natural tissue relaxation allows for the clinical process of stretching—systematically increasing the gauge (thickness) of your jewelry.
Stretching must never be rushed, forced, or attempted blindly at home. The experts at pinktatpier utilize specialized, medically tapered insertion pins to incrementally expand the fistula by a fraction of a millimeter at a time, ensuring the cellular wall remains completely intact without micro-tearing. Upgrading to a heavier, thicker gauge—such as a 6g or 4g—actually increases long-term comfort by further dispersing the physical weight across a wider surface area of the tissue. This professional progression permanently neutralizes any residual “cheese-cutter” risks and heavily enhances the structural stability of the modification.
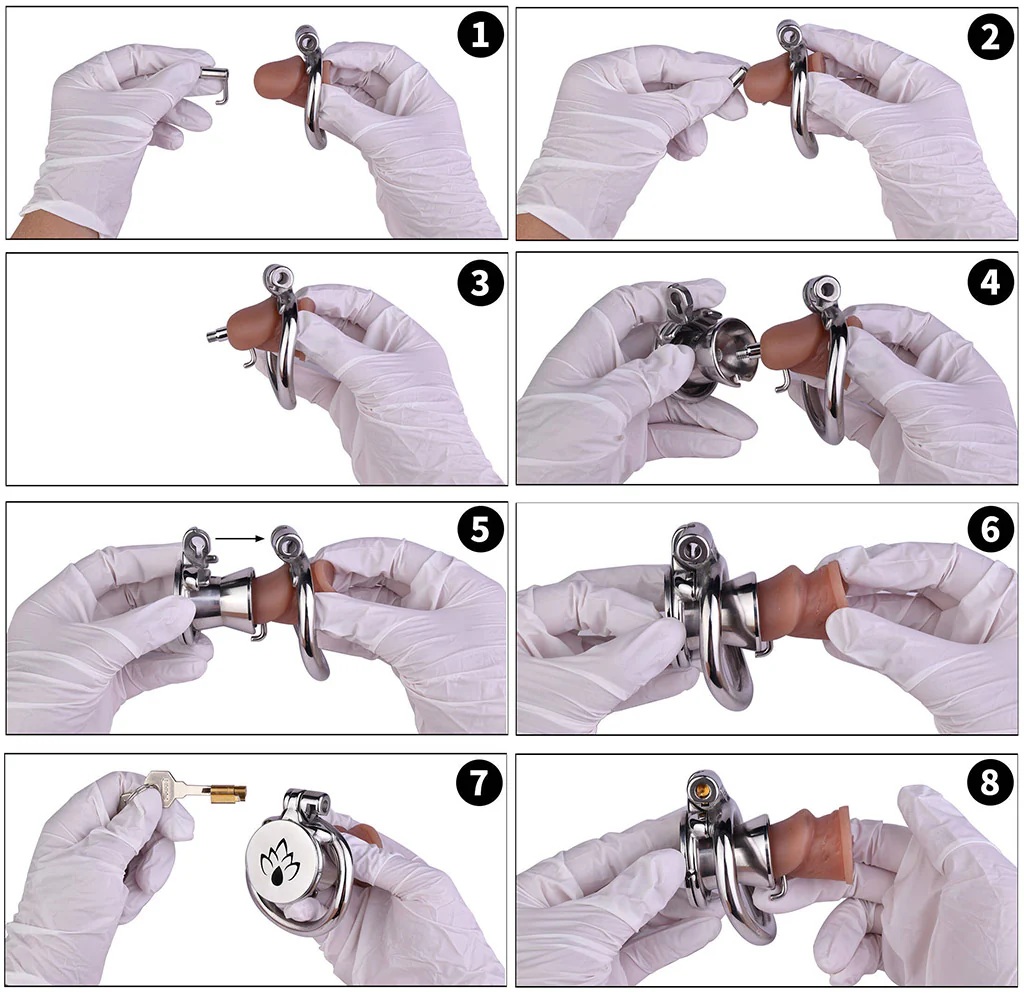
Prince Albert Piercing
Do’s and Don’ts for Intimacy and Sports with a Healing PA Piercing
| Category | Clinical Do’s | Clinical Don’ts |
| Urination | Sit down to urinate to eliminate the “sprinkler effect” mess. | Do not panic if the stream splits; it is structurally normal. |
| Intimacy | Wait a strict 4 to 6 weeks minimum; always use a condom; utilize water-based lubricants. | Do not engage in unprotected or aggressive sexual activity; avoid oil-based lubricants. |
| Athletics | Wear tight, supportive briefs or compression shorts to immobilize the jewelry. | Do not wear loose boxers; do not ride bicycles or horses during the first 8 weeks. |
| Long-Term Care | Have a professional at pinktatpier assess your tissue before attempting a gauge stretch. | Do not forcefully shove larger jewelry into an unyielding or painful channel. |
Frequently Asked Questions (FAQ) and Your Next Steps at pinktatpier
Making the final decision to alter your genital anatomy often brings up highly specific, technical questions that fall outside of standard aftercare or procedural protocols. As you prepare to finalize your journey, it is vital to have absolute clarity on the long-term realities of living with this modification. This concluding chapter addresses the most highly searched, residual queries from our clients, ensuring you are completely equipped with clinical facts before stepping into our state-of-the-art facility.
Closure and Reversal: Will a Prince Albert Piercing Close Up if Removed?
A primary concern for many men is the permanence of the procedure. The reversibility of a Prince Albert modification depends entirely on the chronological maturity of the tissue at the time the jewelry is removed. If the jewelry is taken out during the primary healing phase—specifically within the first eight to twelve weeks—the unkeratinized, highly fragile cellular walls will rapidly collapse. In these early stages, the rich vascularity of the corpus spongiosum will aggressively close the channel, often sealing the puncture completely within a matter of days, leaving only a microscopic, virtually unnoticeable scar.
However, if the piercing has been worn consistently for several years, the internal channel (fistula) becomes a permanent, toughened biological structure. If you choose to permanently retire a fully matured Prince Albert piercing, the visible entry and exit holes will shrink significantly, but the internal tube will likely never fuse back together on its own. Clinically, this means you will be left with a permanent, microscopic patent tract. While it will not look like an open wound, some clients note that during urination, a minute drop of fluid may occasionally seep from the residual exit point at the base of the frenulum. True, total reversal of a deeply established, multi-year genital piercing typically requires a minor, specialized outpatient surgical revision by a urologist to surgically excise the fistula.
Metal Detectors and Medical Scans: Navigating Airport Security and MRIs
For the modern, traveling professional, the logistical implications of carrying specialized internal metal are a highly valid concern. The most frequently asked question regarding travel is: “Will my piercing set off airport metal detectors?” The clinical answer is directly tied to the metallurgical quality of your jewelry. Traditional walk-through metal detectors rely on electromagnetism to detect ferromagnetic materials (metals containing iron, like steel). Because pinktatpier mandates the use of ultra-pure, non-ferromagnetic Implant-Grade Titanium, your jewelry is physically incapable of triggering standard walk-through alarms.
However, advanced airport security now frequently utilizes highly sensitive millimeter-wave body scanners (the machines where you stand with raised arms). These scanners detect physical density anomalies against the natural contour of the human body, regardless of the material. Consequently, a large-gauge titanium ring will register as an anomaly in the pelvic region, which may necessitate a private security pat-down.
In medical settings, the protocols are exceptionally strict. If you require a Magnetic Resonance Imaging (MRI) scan, the powerful magnetic fields mandate the absolute removal of all metallic objects to prevent catastrophic injury, regardless of whether the titanium is technically non-magnetic. Furthermore, metal creates massive visual “artifacts” (bright flares) on X-rays and CT scans, obscuring the physician’s view of your pelvic anatomy. Before any diagnostic imaging, you must temporarily swap your titanium jewelry for a flexible, clinically safe PTFE (Teflon) or glass retainer.
Natural Expansion: Can a PA Piercing Stretch Easily Over Time?
While intentional, manual stretching was addressed previously, clients often wonder if the piercing will simply stretch easily on its own without their intervention. The biomechanical reality is that natural, passive expansion is a guaranteed eventuality for the Prince Albert piercing. The tissue on the underside of the glans is remarkably pliable and gravity-dependent.
When you wear a heavy, solid piece of metal—such as a 6g or 4g Captive Bead Ring—the daily, repetitive micro-movements of walking, combined with the continuous downward gravitational pull, constantly apply gentle tension to the fistula. Over several months to years, the tissue will naturally relax and expand to accommodate this pressure. You will eventually notice that your initial jewelry slides back and forth with zero resistance, and you may even experience slight air or urine leakage around the insertion site. This easy, natural stretching is precisely why starting with a thicker gauge is clinically required; a thin wire would slice through the tissue, whereas a thick ring simply encourages the channel to safely widen. When this natural looseness occurs, visiting a professional to size up your jewelry is recommended to maintain a snug, comfortable fit.
Common PA Piercing Myths vs. Clinical Facts
| The Common Myth | The Clinical Fact |
| “It causes permanent erectile dysfunction.” | False. The piercing strictly traverses the spongy tissue of the urethra, completely avoiding the corpora cavernosa (the primary erectile cylinders). |
| “You can never wear standard condoms again.” | False. Condoms are entirely safe and required during healing. You simply need to ensure the condom is adequately lubricated and rolled over the jewelry carefully. |
| “It will constantly beep at security checkpoints.” | False. Implant-grade titanium is non-ferromagnetic and will not trigger standard electromagnetic walk-through wands or arches. |
| “The piercing will constantly tear during daily life.” | False. When pierced at the correct, thicker gauge (10g or 8g), the weight is perfectly distributed, making structural tearing incredibly rare. |
Booking Your Procedure: Experiencing the Judgment-Free, Expert Environment at pinktatpier
Making the final decision to proceed with a Prince Albert modification is a profound step in personal autonomy. It requires placing immense trust in the practitioner executing the procedure. At pinktatpier, we do not merely perform modifications; we engineer clinical, anatomical enhancements. We understand the deep-seated anxiety, the vulnerability, and the intense psychological buildup that precedes stepping into a studio.
That is precisely why our facility operates under the highest global hygiene standards, mirroring the strict, uncompromising sterility of a medical clinic. Our private, sound-proofed procedural rooms are designed to offer a completely safe, enclosed sanctuary where you can speak openly without fear of judgment, rushed consultations, or unhygienic practices. From the moment you enter, our elite specialists guide you through an empathetic, scientifically grounded process, ensuring every single anatomical variable is accounted for before a needle is ever unwrapped. We replace fear with clinical facts, and apprehension with absolute, unwavering confidence.
Your anatomy deserves nothing less than mastery. Take control of your modification journey today. Contact the specialists at pinktatpier to book your completely private, sterile anatomical consultation, and experience the absolute pinnacle of male piercing safety.








